Removing the Tick
You can’t get sick from a tick that is crawling on you but has not yet attached. Ticks must bite you to spread their germs. If the tick is attached it will be hard to pull off.
Tick attachment time is important. Removing ticks as soon as possible reduces the risk of infection. If you or a loved one is bitten, remove the tick promptly. Here’s how:
- Grasp the tick’s mouthparts against the skin, using pointed tweezers.
- Be patient; the long mouthpart is covered with barbs, so removing it can be difficult and time consuming.
- Pull steadily without twisting until you can ease the tick head straight out of the skin.
- DO NOT pull back sharply; this may tear the mouthparts from the body of the tick and leave them embedded in the skin.
- If this happens, don’t panic! Embedded mouthparts do not transmit Lyme disease.
- DO NOT squeeze or crush the body of the tick; this may force infected body fluids from the tick into the skin.
- DO NOT apply substances such as petroleum jelly, nail polish, or a lighted match to the tick while it is attached. They may agitate the tick and force more infected fluid into the skin.
- Once you have removed the tick, wash the wound site and your hands with soap and water, and apply rubbing alcohol or antiseptic to the site.
- If you have found a tick on you, it’s a sign there may be others. Do a careful tick check.
- Observe the bite site over the next two weeks for any signs of an expanding red rash or flu-like symptoms. (see below)
- Consult with your PCP about sending your tick to a lab, such as TickCheck or TickEncounter, to be tested for pathogens. (see below)
Tick Testing
Consider the utility of sending the tick for identification and analysis of the potential infectious agents of Lyme disease and other tickborne pathogens.
CDC strongly discourages using results from these tick tests when deciding whether to use antibiotics after a tick bite. Positive results can be misleading. Even if a tick contains a pathogen, it does not mean that you have been infected by that pathogen. Negative results can also be misleading. You might have been bitten unknowingly by a different infected tick.
What to do after removing an attached tick that has bitten you.
In general, the CDC does not recomment taking antibiotics prophylactically after tick bites to prevent tickborne diseases. However, in certain circumstances, a single dose of doxycycline after a tick bite may lower your risk of Lyme disease. Consider talking to your healthcare provider if you live in an area where Lyme disease is common to discuss prophylaxic doxycycline and other options.
What to do in the weeks following the tick bite
Recognizing the Rash After a Tick Bite
It is important to understand that a rash is not always present or easily recognizable in early Lyme disease, and this can lead to delayed diagnosis and treatment.
Please refer to our poster of varied Lyme disease rash manifestations as a helpful identification tool.
When present, it is wise to take a picture of the rash with the date for your medical record, since a rash compatible with erythema migrans rash should prompt urgent evaluation and treatment. Lyme disease is most successfully treated in this first stage.
If you have a suspicious rash or your symptoms persist, please seek medical care immediately.
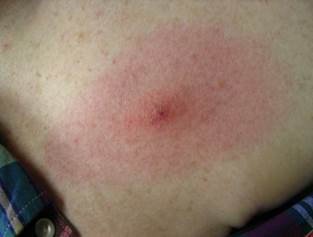
The erythema migrans Lyme disease rash is:
- Round or oval, enlarges in size over days/weeks, & will not fade in a few days
- Usually greater than 2” inches in diameter, often 6-8”
- Usually uniformly red
- Sometimes but not often, a “bull’s eye” rash with a red ring surrounding a clear area and red center
- Minimally tender, minimally itchy (much less itchy than poison ivy), and sometimes warm
- Often confused with spider bites
The incubation period from tick bite to rash is usually 3-10 days but can be 30 days.
The Lyme rash can spread through the bloodstream to other areas of the skin.

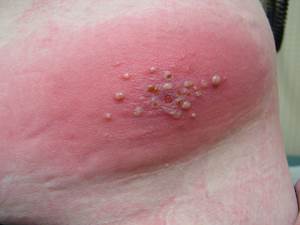
Sometimes blisters develop in the center of the rash.
Tick bite reactions are often confused with the rash of Lyme disease.
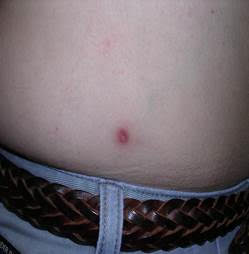
Tick bite reactions:
- Are small red bumps, less than 1-2” in size
- Appear at the site of the bite, often in the groin, belt area, arm pits, or behind the knee
- Do not expand in size when observed over 24-48 hrs
- May feel warm and tender to the touch
- Can last days, even weeks
Requesting and Receiving Care For the Tick Bite
If you have a tick bite, watch for an expanding red rash or lesion at the site of the tick bite or an unexplained feverish, achy, fatiguing illness within 1 to 4 weeks after the tick bite. If you are concerned about symptoms or a rash, take a picture of the rash and contact your physician.
Bitten by a tick and have a rash?
Call our RASH HOTLINE at 410-870-5963 for a rash evaluation appointment.
Diagnosing Lyme Disease:
- Lyme disease is a clinical diagnosis made by a doctor or nurse by examining the patient.
- Acute Lyme disease is not a laboratory diagnosis; a negative Lyme blood test does not exclude Lyme disease in the first few weeks of the illness.
- Many with Lyme disease have a flu-like illness and NO rash.
- Fever, aches, and abrupt and severe fatigue can be the main symptoms of acute Lyme.
- Lyme disease is different from a respiratory “cold”.
- A runny nose and prominent cough are NOT symptoms of Lyme disease.
- Blood tests do not accurately diagnose Lyme disease in the first few weeks of infection, so being vigilant about looking for symptoms is a more reliable way to identify an early case of Lyme disease.
If you have additional questions, please contact your Primary Care Physician or health care provider to discuss.



