
Summary
The erythema migrans (EM) rash, when present, is often the first clinical sign of Lyme disease. This study shows that EM presentations vary with age, sex, EM duration, body location, and timing of initiation of antibiotics. Understanding this EM variability can help physicians and the general public better recognize the rash and improve early diagnosis and treatment.
Why was this study done?
The erythema migrans (EM) skin rash, when present, is often the first clinical sign of Lyme disease. Significant variability in EM presenting characteristics such as shape, color, pattern, and homogeneity, has been reported and could contribute to the misdiagnosis of acute Lyme disease when treatment is crucial. The goal of this research was to analyze the wide variability in EM rash presentations by studying associations between EM rash characteristics, as well as examining whether the varied presentations were associated with age, sex, EM duration, body location, and initiation of antibiotics.
How was this study done?
The study enrolled two hundred and seventy one adult participants with early Lyme disease who had a physician-diagnosed EM skin lesion of ≥ 5 cm in diameter and ≤ 72 hours of antibiotic treatment. Participant demographics, clinical characteristics, and characteristics of their primary EM lesion were recorded and analyzed.
What were the major findings?
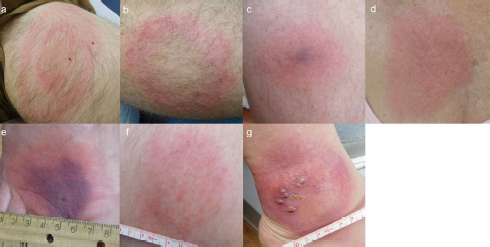
Results showed that EM presentations vary with age, sex, EM duration, body location, and initiation of antibiotics. Major findings include:
After adjusting for potential confounders, the EM rash size increased along with increasing duration to a peak of 14 days.
Male EM were found to be on average 2.18 cm larger than female EM.
The odds of a red (vs blue/red) EM were 65% lower in males compared to females.
The odds of a red (vs blue/red) EM were over 3 times as high if found on the pelvis, torso, or arm compared to the leg.
Compared to EM on the leg, those on the pelvis or torso were approximately 2.5 times as likely to be oval than round, and those who had initiated antibiotics were 49% less likely to have an oval EM than a round one compared to those who had not initiated antibiotics.
Age remained a significant predictor of central clearing in adjusted models; for every 10-year increase in age, the odds of central clearing decreased 25%. The older the participants the lower their odds of having a “bulls-eye” rash with central clearance.
What is the impact of this work?
Given that EM remains a clinical diagnosis for Lyme disease, it is essential that both physicians and the general public are aware of its varied presentations, especially since misdiagnosis is known to be a problem. Most physicians are aware of the association of the bulls-eye rash to Lyme disease but may not be aware that the bulls-eye rash is not the most common EM rash presentation. This research improves the understanding of the varied clinical spectrum of EM and suggests possible patterns within this variability which have implications for early diagnosis and treatment.
Support:
This work was supported by a subagreement from the Johns Hopkins University with funds provided by a Grant Agreement from the Steven and Alexandra Cohen Foundation. Support was also provided from the Global Lyme Alliance (GLA) and the Bay Area Lyme Foundation (BALF). This publication was also made possible by the Johns Hopkins Institute for Clinical and Translational Research (ICTR), which is funded in part by Grant Number UL1 TR003098 from the National Center for Advancing Translational Sciences (NCATS) a component of the National Institutes of Health (NIH), and NIH Roadmap for Medical Research, and the Johns Hopkins Clinical Research Network (JHCRN).
Publication Information
Rebman, A.W., Yang, T., Mihm, E.A. et al. The presenting characteristics of erythema migrans vary by age, sex, duration, and body location. Infection (2021). https://doi.org/10.1007/s15010-021-01590-0


